How Hospitals Can Reduce RSV, Flu, and COVID Transmission During Emergency Department Surges
Emergency departments across the country are facing unprecedented pressure. Seasonal respiratory illnesses such as RSV, influenza, and COVID-19 continue to strain hospital capacity, while overcrowding and hallway care have become routine in many facilities.
When patient volumes spike, hospitals must quickly create additional treatment zones while maintaining strict infection control standards, patient privacy, and regulatory compliance. Unfortunately, many traditional privacy solutions—especially fabric curtains—were never designed to support modern surge conditions or airborne pathogen control.
Today, hospitals are increasingly turning to medical-grade partition systems that provide rapid deployment, non-porous surfaces, and flexible patient separation. These solutions help emergency departments create safer environments during respiratory outbreaks while supporting operational efficiency and regulatory readiness.
This article explores how modern medical partition systems can help healthcare leaders manage infection control, surge capacity, and patient flow during RSV, COVID-19, and influenza events.
The Growing Challenge of ER Overcrowding
Emergency department overcrowding has become one of the most significant operational challenges facing hospitals today.
Common contributors include:
- Seasonal respiratory virus outbreaks
- Hospital bed shortages
- Emergency department boarding
- Rising patient volumes
- Limited surge infrastructure
When inpatient beds are unavailable, patients are often treated in hallways or overflow areas, creating significant challenges for infection prevention teams.
Risks associated with hallway care include:
- Lack of physical patient separation
- Increased cross-contamination risks
- Reduced patient privacy
- Higher exposure for staff and visitors
- Difficulty maintaining infection control protocols
Without effective physical barriers, airborne and droplet pathogens can easily spread within crowded emergency departments.
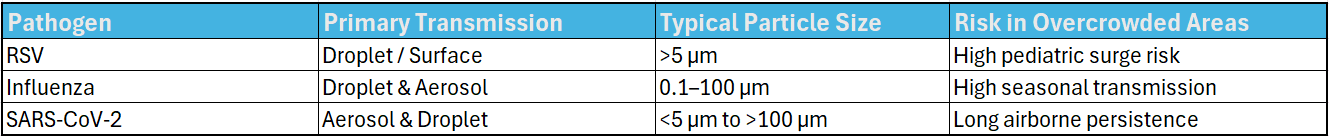
Understanding Respiratory Virus Transmission in Hospitals
Respiratory viruses spread primarily through droplets, aerosols, and contaminated surfaces.
Below is a simplified overview of the most common pathogens affecting emergency departments.
During coughing, sneezing, or talking, infected patients release respiratory droplets that can travel several feet and remain suspended in the air.
In crowded emergency departments, this can lead to:
- Rapid patient-to-patient exposure
- Staff contamination risks
- Surface contamination on nearby equipment
- Environmental viral persistence
Effective infection control requires interrupting these transmission pathways.
Why Traditional Hospital Curtains Create Infection Risks
For decades, hospitals have relied on fabric privacy curtains to separate patients. However, growing evidence shows that these curtains can become significant reservoirs for pathogens.
Studies have found that hospital curtains can become contaminated with bacteria such as MRSA or VRE within 7–14 days of installation.
This happens because fabric surfaces:
- Absorb respiratory droplets
- Trap microorganisms within fibers
- Are difficult to disinfect quickly
- Are touched frequently by staff and patients
Additionally, fabric curtains are often difficult to deploy in hallways, temporary treatment areas, or surge spaces where ceiling tracks are unavailable.
As emergency departments increasingly rely on temporary treatment zones, hospitals need more flexible infection control barriers.
The Role of Medical Partition Systems in Infection Control
Modern medical partition systems provide an alternative approach to patient separation. These systems use non-porous, wipeable surfaces designed for rapid disinfection and flexible deployment.
Key benefits include:
Non-Porous Infection Control Surfaces
Medical-grade surfaces allow staff to disinfect barriers using standard hospital disinfectants such as:
- Quaternary ammonium compounds
- Hydrogen peroxide solutions
- Sodium hypochlorite (bleach)
- Clinical wipes such as CaviWipes or Sani-Cloth
Unlike fabric curtains, non-porous surfaces do not absorb infectious droplets, allowing pathogens to be removed quickly.
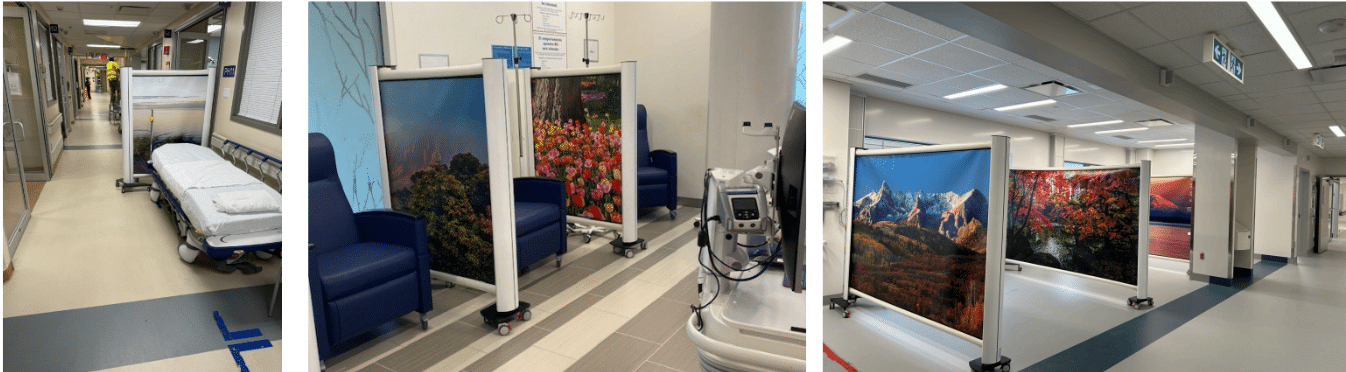
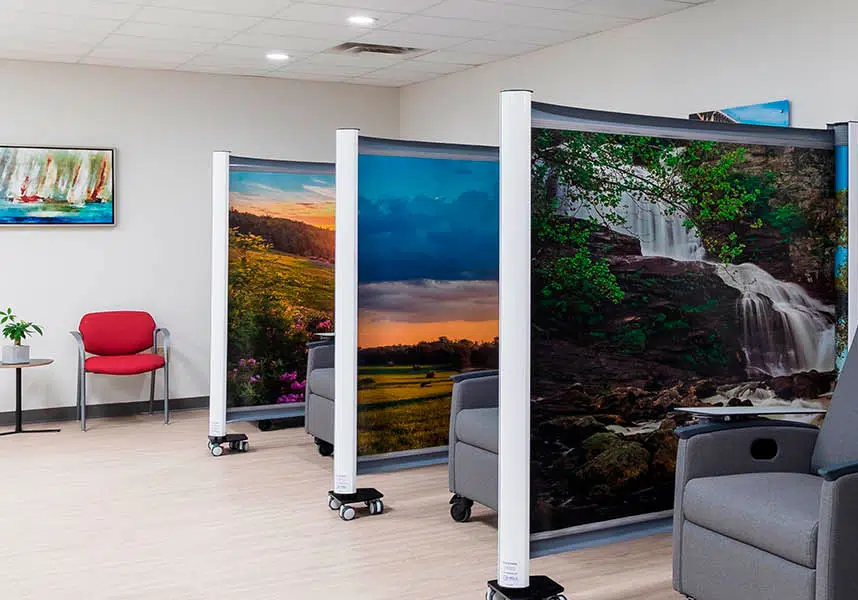
Rapid Surge Deployment
Portable medical partition systems allow hospitals to create instant treatment zones in areas such as:
- Emergency department hallways
- Waiting rooms
- Temporary triage areas
- Converted conference rooms
- Vaccination clinics
- Overflow patient spaces
In many cases, a single staff member can deploy a partition system in seconds, allowing facilities to respond quickly to unexpected patient surges.
Patient Cohorting During Respiratory Surges
During outbreaks of RSV, influenza, or COVID-19, infection control teams often use cohorting strategies to separate symptomatic patients from others.
Medical partition systems allow hospitals to quickly create:
- Respiratory isolation zones
- Pediatric RSV treatment areas
- Dedicated respiratory waiting areas
- Temporary exam bays
These physical barriers help reduce direct exposure between patients.
Improving Emergency Department Workflow
Beyond infection control, partition systems can improve overall emergency department workflow.
Benefits include:
- Faster room turnover
- Improved patient privacy
- Better organization of hallway treatment areas
- Reduced noise and visual distractions
- Clear separation between patient care zones
For nursing teams managing high patient volumes, these systems can help create more structured care environments during peak demand periods.
Supporting Compliance with Healthcare Safety Standards
Hospitals must maintain strict environmental safety standards set by organizations such as:
- The Joint Commission
- OSHA
- CMS
- NFPA
These agencies emphasize:
- Infection prevention practices
- environmental hygiene
- patient privacy
- staff safety
Medical partition systems can support these goals by providing cleanable surfaces and flexible infrastructure for infection control procedures, particularly during surge events when traditional treatment spaces become limited.
The Financial Impact of Infection Prevention
Hospital-acquired infections (HAIs) carry significant clinical and financial consequences.
Healthcare organizations face:
- Increased treatment costs
- extended hospital stays
- regulatory penalties
- reduced patient satisfaction scores
- potential reimbursement impacts
Investments in infection prevention infrastructure can help hospitals reduce these risks while improving operational efficiency.
Preparing for the Next Respiratory Surge
Respiratory virus seasons will continue to challenge healthcare systems. RSV, influenza, and emerging pathogens can quickly overwhelm emergency departments if facilities lack flexible infrastructure.
Hospitals that invest in adaptable infection control solutions are better positioned to:
- manage patient surges
- protect healthcare workers
- maintain patient safety
- improve operational resilience
Modern medical partition systems represent one of the practical tools hospitals can use to support surge readiness and infection control in today’s healthcare environment.
Emergency departments must balance patient care, infection prevention, and operational efficiency during periods of extreme demand. As respiratory illnesses continue to drive hospital surges, healthcare leaders are reevaluating traditional infrastructure approaches.
Medical partition systems offer a modern solution that supports infection control, rapid space creation, and improved patient separation during RSV, flu, and COVID-19 outbreaks.
By integrating flexible barrier systems into their emergency preparedness strategies, hospitals can strengthen their ability to respond to both seasonal surges and future public health emergencies.
Contact us today to schedule a workspace assessment or request a custom quote.
FAQs
How do hospital partition systems help control infection spread?
Medical partition systems create physical barriers between patients, helping reduce exposure to respiratory droplets and contaminated surfaces. Their non-porous materials allow rapid disinfection, which supports infection prevention protocols in busy clinical environments.
Why are traditional hospital curtains considered infection risks?
Fabric curtains can absorb respiratory droplets and harbor bacteria or viruses within their fibers. Because they are difficult to disinfect quickly, they can become reservoirs for pathogens in high-traffic healthcare settings.
Can medical partition systems be used during emergency department overcrowding?
Yes. Portable partition systems can quickly create temporary treatment spaces in hallways, waiting rooms, or overflow areas, helping hospitals maintain patient separation during surges.
What types of viruses can hospital partition systems help mitigate?
Physical barriers help reduce exposure risks from respiratory pathogens such as:
- RSV
- Influenza
- COVID-19
- Other droplet or aerosol transmitted viruses
While barriers alone do not eliminate infection risk, they complement broader infection control strategies.
How quickly can medical partitions be deployed in hospitals?
Most modern portable partition systems can be deployed in seconds by a single staff member, making them ideal for surge events or temporary treatment areas.